Why bone health after 50 demands more than easy fixes
05/09/2026 / By Ava Grace
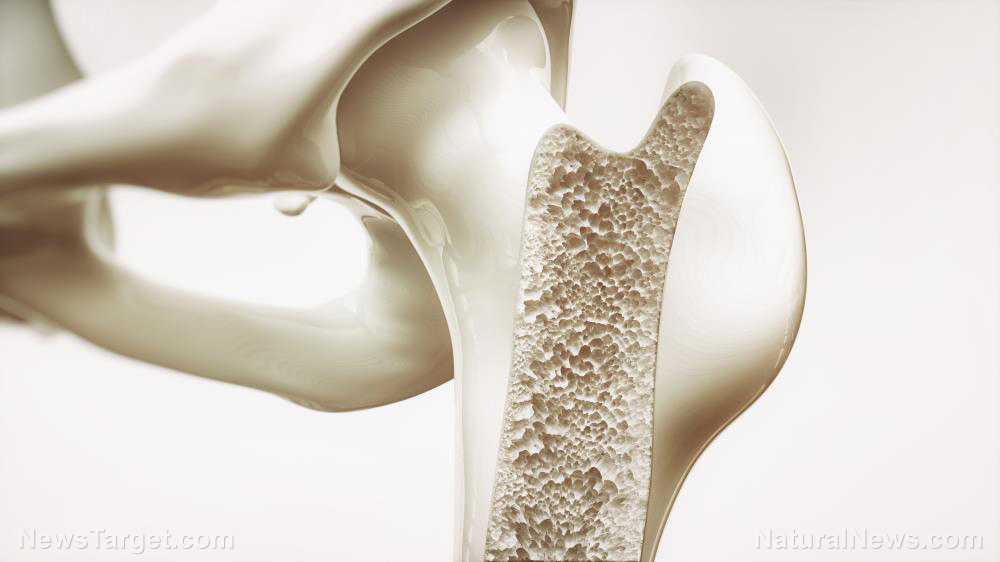
- After age 50, particularly for women post-menopause, the body loses bone faster than it builds it, leading to osteoporosis. This silent process increases fracture risk, loss of height and disability, demanding serious attention.
- While calcium and vitamin D are essential, a truly bone-protective diet requires a full spectrum of nutrients—including protein, magnesium and vitamins K and C—primarily from whole foods like leafy green vegetables.
- Smoking and excessive alcohol consumption are proven, direct causes of decreased bone density and increased fracture risk, representing clear areas where personal choice can alter health outcomes.
- Bones require stress to maintain density. Weight-bearing and resistance exercises are crucial medicine, providing the mechanical signal to build bone and improve muscle and balance to prevent falls.
- For those with bone loss, preventing falls is imperative. This requires proactive environmental modifications (like grab bars and clear walkways) and, if needed, using assistive devices to avoid life-altering fractures.
In an era of simplified health advice and listicle-driven wellness, a critical message about aging is being diluted into palatable, risk-free tips. The stark reality of bone health after age 50, a physiological turning point for millions, is often glossed over with generic recommendations that ignore the hard truths of biology and personal responsibility. This matters now more than ever, as an aging global population faces a looming crisis of osteoporosis and fragility fractures, conditions that steal independence, drain healthcare resources and diminish quality of life. The conversation must move beyond “easy ways” to confront the actionable, sometimes difficult, changes required to fortify the skeleton against the inevitable wear of time.
The unavoidable calculus of aging
The human skeleton is not a static scaffold but a living, dynamic organ constantly remodeling itself. After age 50, particularly for women post-menopause, this balance shifts decisively toward loss.
“The sharp decline in estrogen after menopause accelerates bone loss by increasing osteoclast activity,” said BrightU.AI‘s Enoch. “This hormonal shift tips the natural bone remodeling equilibrium further, causing bone breakdown to outpace formation at a much faster rate. The cumulative effect of this imbalance, which begins around age 35, becomes significantly more pronounced, leading to accelerated bone density loss.”
The body reabsorbs old bone faster than it creates new bone, leading to a decline in bone mineral density. This process, often silent until a fracture occurs, is the foundation of osteoporosis, a condition that renders bones porous and brittle. The spine compresses, posture stoops and height diminishes. This is not mere vanity; it is a structural compromise that alters the center of gravity and increases fall risk, setting the stage for a cascade of disability.
Nutrition: Beyond the calcium quick-fix
Conventional wisdom shouts about calcium and vitamin D, and for good reason. Calcium is the primary mineral in bone, and vitamin D, synthesized through skin exposure to sunlight, is its essential partner for absorption. However, a conservative, clear-eyed view of nutrition reveals this as a necessary but insufficient baseline. The modern diet, often deficient in whole foods, fails to deliver a symphony of other crucial nutrients. Protein and collagen provide the bone matrix; magnesium aids in calcium incorporation; and vitamins K and C are vital for bone protein formation and antioxidant protection. A diet lacking in vegetables—particularly the leafy greens and cruciferous varieties like spinach and broccoli—deprives bones of the compounds that shield them from cellular damage and support mineralization. Severe calorie restriction, often pursued for weight loss, can backfire catastrophically, triggering muscle wasting and further bone density loss.
The toxins we choose: Smoking and alcohol
Research has unequivocally drawn a line between tobacco use and decreased bone density. The toxins in smoke disrupt the bone remodeling cycle, poison bone-forming cells and impair healing. The result is a significantly higher risk of fracture, especially of the hip—a devastating injury. Similarly, excessive alcohol consumption interferes with bone remodeling and nutrient balance. Perhaps more insidiously, it increases the risk of falls, creating a perfect storm for fracture. These are not vague correlations but direct consequences of individual habit, areas where sheer personal resolve can alter a health trajectory.
Bones rebuild in response to stress. A sedentary life is a prescription for accelerated bone loss. Conversely, physical activity, particularly weight-bearing and resistance exercises like walking, lifting weights, or using resistance bands, provides the mechanical signal bones need to maintain density and strength. High-intensity resistance training has shown particular promise. This is not about vanity but structural integrity. Furthermore, exercise improves muscle mass, coordination and balance, directly combating the leading cause of bone-breaking trauma: falls.
The fall prevention imperative
Preventing falls is a non-negotiable pillar of bone health. This requires a clear-eyed assessment of one’s environment: installing grab bars in bathrooms, ensuring stairways have handrails on both sides, and keeping walkways free of clutter. It also underscores the critical importance of using prescribed orthotic devices after an injury to stabilize joints and allow proper healing, preventing re-injury.
The path to prioritizing bone health after 50 is less about discovering “easy ways” and more about embracing a sustained commitment to foundational health principles. This is a conservative approach in the truest sense: it conserves the body’s natural capital through proactive, evidence-based stewardship. The truth is that strong bones in later life are not an accident of genetics alone but the reward for a lifetime of conscious choices, a reward that preserves strength, autonomy and dignity.
Watch this video about the book “Nutrition and Bone Health” by Dr. Michael Holick and Dr. Bess Dawson-Hughes.
This video is from the BrightLearn channel on Brighteon.com.
Sources include:
Submit a correction >>
Tagged Under:
Alcohol, bone density, bone health, natural cures, natural medicine, remedies, research, resistance training, sedentary life, smoking, stress
This article may contain statements that reflect the opinion of the author
RECENT NEWS & ARTICLES
COPYRIGHT © 2017 TOXINS NEWS